Proper Diagnosis of Non-restorable Tooth Fractures
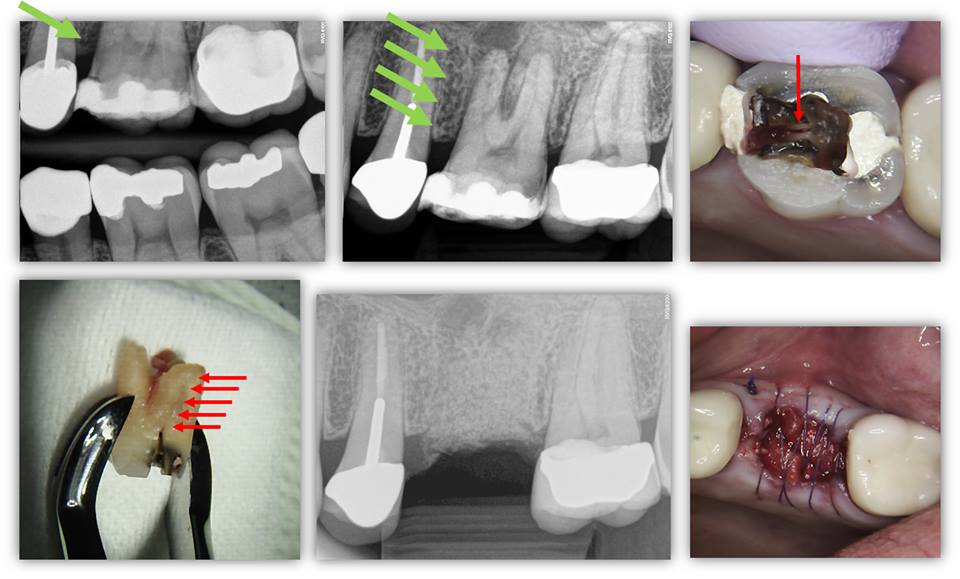
PROPER DIAGNOSIS OF NON-RESTORABLE TOOTH FRACTURES: This patient presents to our office with attempted excavation of an existing restoration and to evaluate the extent of a fracture in the crown (the patient had an MOD composite restoration). It was known by the restorative dentist that the tooth was necrotic (Note MB root lesion). For whatever reason, the dentist decided at this point to temporize and send to us for case management. BEFORE clinical exam and considering CBCT, we had noted several key factors in the PA and BW radiographs; the most important facto was the presence of bone loss on the mesial aspect of the tooth as evidenced by the green arrows. This would be highly suggestive that the crown fracture traverses below both CEJ and level of the alveolar crest. This is because bacteria populates into the fracture causing a localized inflammatory response and resultant bone loss (green arrows). Interestingly, this case didn’t probe even under pressure (this is possibly because the placement of the probe wasn’t at the exact angle of the bony defect). In any case, the patient was informed that this was not a restorable situation and it was decided that a dental implant would be done (the adjacent crowns were deemed adequate and there was no plan for replacement despite a slight distal overcontour of #14). For the sake of exercise and curiosity, the tooth was endodontically accessed to reveal a fracture that traverses the pulp chamber floor. Upon extraction, the root fracture spanned the entire length of the MB root (red arrows). The tooth was extracted and grafted for future dental implant placement. To all my endodontist colleagues out there, who would have taken a CBCT on this case for the purpose of pre-operative diagnosis? Although we will eventually be taking a CBCT on this particular patient in preparation for the dental implant, we did not take one for diagnosis and planning for extraction/site preservation.