WHAT EXACTLY IS MODERN SURGICAL ENDODONTICS?
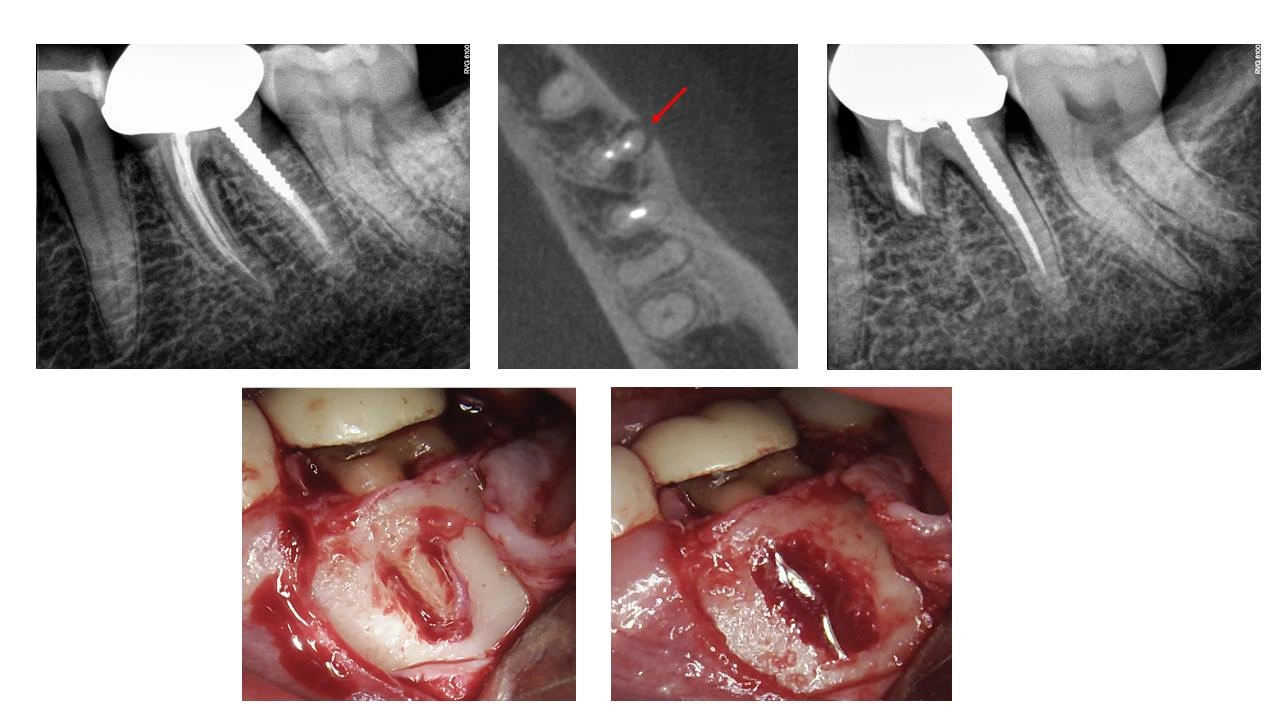
Speaking with classically trained oral surgeons, many dentists are under the impression that an apicoectomy is a ’50/50′ procedure. Until the recent advent of CBCT, ultrasonics, and microscope aided surgical therapy, they’d be absolutely right. However, these tools have drastically changed the landscape and success rates of surgical endodontics. The case below illustrates two key features: (1) On pre-operative PA, you would be hard pressed to point out a lesion despite the patient’s pain; however, CBCT clearly demonstrates pathosis on the buccal surface of the mesial root (red arrow) that, for obvious reasons of superimposition, won’t show up on a 2D PA image. (2) Upon elevating a flap, a buccal root fracture was confirmed as suspected. However, because the fracture started apically and progressed coronally (as demonstrated by a sound 3 mm collar of coronal buccal cortical plate which we could see on CBCT), we were able to slowly resect the root under extremely high magnification using the microscope until the fracture was completely removed. The crown/root ratio is clearly compromised on the mesial root, but this is relatively meaningless in a multirooted tooth as long as a 3 mm collar of cortical plate remains. Using modern microsurgical techniques, we were able to save a tooth that would traditionally follow the path of “I don’t know why you’re in pain. Your tooth is probably fractured, lets just pull it and place an implant” which for this patient is hugely advantageous given their particular medical history.